As the U.S. population ages, addressing the complex mental health needs of seniors is rapidly shifting from a niche social concern to a central pillar of healthcare policy. For decades, geriatric mental health was a fragmented, marginalized sub-sector of the broader healthcare market. Today, it has emerged as a central economic and policy imperative. The intersection of an aging population, rising clinical acuity, and major regulatory catalysts have driven senior mental health care into a centralized focal point of investment activity. Investors have a unique opportunity to capitalize on the transition from fragmented, facility-based care to integrated, technology-enabled, and differentiated care delivery models.
Aging Demographics & The Mental Health Crisis
The landscape of the senior mental health industry is being reshaped by demographic trends, particularly the rapid expansion of the aging population. The population of people aged 75 and older is projected to grow at nearly 4% annually and reach over 33 million by 2030. More broadly, the number of Americans aged 65 and older is projected to increase from 58 million in 2022 to 82 million by 2050. The baby boomer generation will soon make up nearly a quarter of the total U.S. demographic.
This population shift is accompanied by a sharp rise in the frequency of serious mental health concerns that require medical intervention. Approximately 25% of seniors suffer from depression and anxiety, which often manifest as physical symptoms that drive high medical utilization. Additionally, substance use disorders (SUDs) are becoming a significant issue, with alcohol use disorder affecting roughly 5% of older adults and opioid misuse remaining a persistent threat due to chronic pain management. Cognitive decline further compounds these challenges, as greater than 7 million Americans are living with Alzheimer's and dementia today; this number is projected to rise to nearly 13 million by 2050.
Beyond diagnosable psychiatric conditions, social isolation has emerged as a severe clinical indication: approximately 33% of older adults reported feeling lonely in 2024, a condition that carries a mortality risk comparable to smoking and drives higher rates of heart disease and stroke. These overlapping physical and behavioral health challenges are particularly severe in long-term care settings, where notably, over 75% of individuals have multiple chronic conditions. As these numbers climb, there is an urgent need to increase access to high-quality geriatric mental health care tailored to the complex needs of older adults.
Overall, the trends are persistently clear. Americans are not just aging rapidly, but they’re burdened by a myriad of increasingly complex medical, behavioral, and social ailments - all of which require targeted care for adequate treatment.
Regulatory Initiatives & Medicare Reimbursement Reform
As national recognition grows that mental health is inseparable from physical health, the Centers for Medicare and Medicaid Services (CMS) is modernizing its frameworks to support more holistic care for seniors. A meaningful step forward is the introduction of new Medicare billing codes for Digital Mental Health Treatment (DMHT) in the 2025 Medicare Physician Fee Schedule, which allows healthcare providers to integrate digital therapeutics into their patients' daily lives. To address severe clinician shortages, recent workforce initiatives (effective January 1, 2024) unlock over 400,000 additional providers by allowing Marriage and Family Therapists (MFTs) and Mental Health Counselors (MHCs) to independently bill Medicare Part B for the diagnosis and treatment of mental illnesses. Furthermore, these updated regulations now permit MFTs and MHCs to offer Health Behavior Assessment and Intervention (HBAI) services, bill separately from Skilled Nursing Facility consolidated billing, and serve on hospice interdisciplinary teams.
Beyond expanding the provider base, CMS is also investing into initiatives that seek to incorporate coordinated care models, wherein mental health becomes a key element of overall care delivery. A cornerstone of this effort is the Guiding an Improved Dementia Experience (GUIDE) Model, an eight-year initiative launched on July 1, 2024, which tests per-beneficiary-per-month payments for comprehensive dementia care management. The program aims to improve the quality of life for seniors and reduce unnecessary hospitalizations by funding dedicated care coordination, 24/7 support line access, and caregiver education. This specialized focus has manifested in the broader maturation of Behavioral Health Integration (BHI) services. Initially launched in 2017 to support mental health and psychiatric conditions in primary care, BHI has evolved over the last decade into a vital framework for senior care settings, allowing providers to weave mental health support directly into daily clinical workflows. Furthering this momentum, CMS announced the Innovation in Behavioral Health (IBH) Model in January 2024. Following a pre-implementation phase that began on January 1, 2025, the model is set for full implementation starting January 1, 2028, focusing on specialized, community-based care by connecting specialty practices with physical healthcare and social services to address moderate-to-severe conditions.
These initiatives reflect a broader transition toward value-based care. Programs such as the Medicare Shared Savings Program (MSSP) and the ACO REACH model incentivize providers to assume financial accountability for their patients' complete health. Numerous post-acute organizations (including Eventus, LTC ACO, Palm Beach ACO, Sound Physicians, TeamHealth, and Theoria, to name a few), have embraced these frameworks by launching their own ACOs to better manage the total cost and quality of care for older adults in post-acute settings. These organizations collectively delivered hundreds of millions of dollars of savings in 2024 alone. Within the REACH model specifically, High Needs ACOs focused on complex populations have achievedTotal Quality Scores of 86.7% and net savings rates of 13.2%, significantly outperforming the overall REACH model averages of 79.4% and 4.1%, respectively.
New and Emerging Sites of Care
Long-term care communities, such as skilled nursing facilities and assisted living facilities, are evolving into fully integrated care sites where providers deliver onsite behavioral health services. Beyond facility walls, the overwhelming preference among older adults is to age in place, driving the expansion of "hospital-at-home" models. As acute medical care moves into the home, adding a behavioral layer, such as embedded psychiatric consults for seniors with dementia, is essential to prevent readmissions. To further bridge access gaps, mobile behavioral health units are operating as "clinics on wheels", bringing interdisciplinary teams of social workers, peer specialists, and paramedics directly to seniors with mobility challenges to de-escalate crises on-site, avoiding law enforcement involvement and emergency room visits. Finally, the extension of Medicare telehealth flexibilities, particularly audio-only appointments through 2026, remains a critical lifeline for reaching immobile seniors.
In rural care deserts, Critical Access Hospitals have emerged as essential mental health hubs, launching geriatric intensive outpatient programs that deliver high-quality, local therapy for depression, anxiety, and loneliness. To address the severe nationwide shortage of specialized clinicians, many rural hospitals partner with outsourced providers such as Psychiatric Medical Care, UltraGroup Healthcare, Signet Health, and Horizon Health. These partners provide comprehensive, turnkey solutions, including supplying licensed therapists, remote psychiatrists, and compliance oversight, to ensure that rural populations have access to essential mental health services.
Investment Interest in Assets Focused on Senior Mental Health
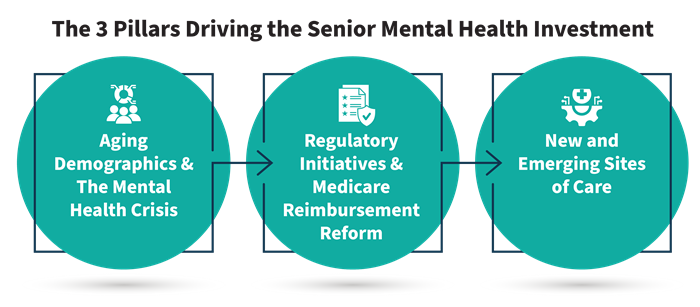
The growing recognition of this crisis has accelerated investment from private equity and behavioral health consolidators seeking to address the widening supply gap for geriatric behavioral health services. Highlighted below are select recent investments made in companies providing specialized solutions to serve the aging population:
Future Outlook - The Senior Mental Health Opportunity
The convergence of unprecedented demographic growth, deepening severity of geriatric mental health needs, and supportive Medicare and regulatory reform has created a unique opportunity for companies and investors to help bridge the gap between clinical scarcity and the rising demand for specialized geriatric mental health services. These tailwinds are driving a shift in how geriatric care is delivered as the market moves away from fragmented, reactive institutional care toward integrated, collaborative models delivered in familiar patient settings. This transition is essential to effectively managing a highly complex patient population that often deals with co-existing physical and mental health conditions.