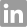The Third-Party Administrator (TPA) market is undergoing transformation. The category has increased in importance over the past several years driven by an accelerating shift towards employer self-funding and a growing demand for highly customized, flexible, and cost-effective healthcare benefits solutions. TPAs have evolved from traditional claims processors into more sophisticated platforms that both deliver proprietary value-added benefits services and act as an integrator for important point solutions.
TPAs are becoming a critical lever to address healthcare spend and are taking on a new identity as they seek to expand on ROI-driven services. As capital continues to flow into TPA strategies and well funded platforms seek ways to differentiate in the market, we expect the next generation of successful TPAs to possess several of these critical attributes:
- Technological Sophistication: Robust, scalable technology platforms for claims processing, data management, and member engagement. Investments in AI to stay competitive, build operational efficiencies, enhance the member experience, and identify cost savings opportunities
- Advanced Analytics: Ability to provide deep, actionable insights into healthcare utilization and costs
- Strong Vendor Relationships: A curated ecosystem of high-quality, integrated point solutions
- Client-Centricity & White-Glove Service: A commitment to exceptional service and customized solutions that meet evolving employer needs
- Scalability: The infrastructure and operational capabilities to grow efficiently with increasing demand
- Proprietary Cost Containment Capabilities: Ownership of or deep partnerships for advanced cost management strategies
New Value Propositions are Emerging
The roadmap for TPAs to extend their value proposition is coming into focus, anchored by the type of cost containment strategies that deliver the strongest ROI, with the goal of positively impacting overall healthcare spend. Some organizations are finding success building capabilities in-house, while others are seeking strategic partnerships that can advance a more integrated and flexible model.
TPAs are in a unique position in the self-funded ecosystem. In an employer’s pursuit of a more customized benefit plan, TPAs have emerged as a key enabler to support and craft a strategy alongside an employer’s benefits broker. This placement presents the opportunity for the TPAs to expand their value proposition, including the ability to impact cost and generate new fee opportunities. With medical inflation registering over 8% in 2025 and 2026, employers have become much more open to exploring new and more aggressive cost containment alternatives.
Several categories have emerged as important levers to impact plan spend, healthcare quality, and overall member experience. Plan administrators are expanding their capabilities and partnerships in these categories to be able to offer robust solutions to their employer clients.
Strategies Emerging for Next Generation TPAs
There are tangible examples of companies unlocking value with thoughtful, integrated strategies that align to their current structure and size. Primary care, proprietary networks, and integrated navigation are all individually being tested as second cornerstones to a robust administration function in positioning what a next generation TPA could be.
Primary Care Driven Models – This strategy focuses on primary care as a critical entry point to the healthcare system, establishing that point of engagement as a key component to controlling healthcare costs and managing towards a positive member experience. Select TPAs are leaning into primary care networks to improve utilization and navigation to quality specialty care; supplementing with tools to engage virtually. With this model, TPAs are developing new offerings that include changes to benefit design, like low/no deductibles and limited co-pay for select services, that are attractive to both employees and employers.
Proprietary Networks – With a track record of driving significant and immediate cost savings, this strategy directly addresses the overall inflated nature of contracted rates within broad PPO networks. This strategy takes over all critical functions that a traditional health plan may offer, with a message of a fully integrated offering delivering stronger cost savings than health plans can offer. These network strategies can be complete open access or involve a narrow network supplemented by a wrap network (often for professional/non-facility claims) or reference-based OON re-pricing. This requires robust member services, provider relations capabilities, advanced claim adjudication and routing, deep data experience and infrastructure, and appeal defense. The integration of these two models, which often are partners, is driven by the importance of controlling the full member experience while maximizing savings.
Member Navigation – This strategy is focused on maximizing the proper utilization of the best parts of the TPA unbundled benefit plan through effective navigation solutions that engage individuals to manage the cost, quality, and experience of care. These platforms have developed the DNA to engage individuals and help them make the right healthcare decisions. They often combine the user experience of an advanced technology platform with strong member service elements of a TPA. AI will increasingly become an important element of this strategy. TPAs with navigation solutions can leverage AI to orchestrate the patient journey by triaging symptoms, scheduling care, and closing care gaps without manual intervention.
Additional Growth Tailwinds Supporting TPA Adoption
The emergence of various alternative funding solutions is helping open doors for smaller employers to consider different forms of self-funding, in turn creating new opportunities for TPAs. Captives and level-funded vendors are opening a channel to <250 life employer groups, all of which require effective TPA solutions to operate their benefit plan strategies in the way they intend. These categories are some of the fastest growing in the self-funded landscape, presenting a beneficial tailwind to the growth of the segment. TPA platforms that align to fast growing vendors in these respective spaces are creating a new and highly effective growth channel.
Health Plans and the Competitive Environment
Expanding interest on the part of small and mid-size employers in exploring TPAs and unbundled solutions has forced health plans to think more critically about how they can offer more customized solutions to the market. Plans have often struggled to serve the small and mid-size employer market with the flexibility being demanded, often defaulting to rigid plan structures that emphasize the plan’s in-house solutions. However, recognizing the shifting demands of the market, health plans have been active acquirers for leading independent TPAs looking to defend their regional territories and acquire the expertise to deliver a more customized experience. Managed care organizations like HCSC, Elevance, BlueCross BlueShield of North Carolina, and UnitedHealth Group have all made recent acquisitions in the TPA market to fortify their positions and remain competitive among their peers.
The Future is Coming Into Focus
The investment landscape for Third-Party Administrators remains incredibly vibrant, characterized by a healthy M&A environment and robust interest from financial sponsors. As the market evolves, strategic interest is increasingly filtered through the lens of a TPA’s unique capabilities and specialized solutions, geographic presence and the infrastructure to serve members at significant scale. Ultimately, as capital continues to flow into the sector, the best valuations will be reserved for TPA platforms that demonstrate a powerful combination of top-line growth, high client retention, and the operational strength to scale efficiently in a complex healthcare ecosystem.
TripleTree is committed to sharing the most relevant industry insights and trends that are impacting the healthcare market. Read more of our recent insights today or connect with us at an upcoming industry gathering: