As government’s role in the provisioning of health care and welfare benefits continues to increase, the number of participants in state administered benefit programs and the burden of supporting those programs is also growing. Anti-poverty spending as shown in the graph below, has reached 4% of GDP, of which healthcare entitlement programs represent more than 1.5% (and is speculated to be the largest risk of runaway spending). Given the demographics of the low-income population served by these programs, a high level of duplicative efforts are taking place on a state administrative level in order to manage and administer these benefits.
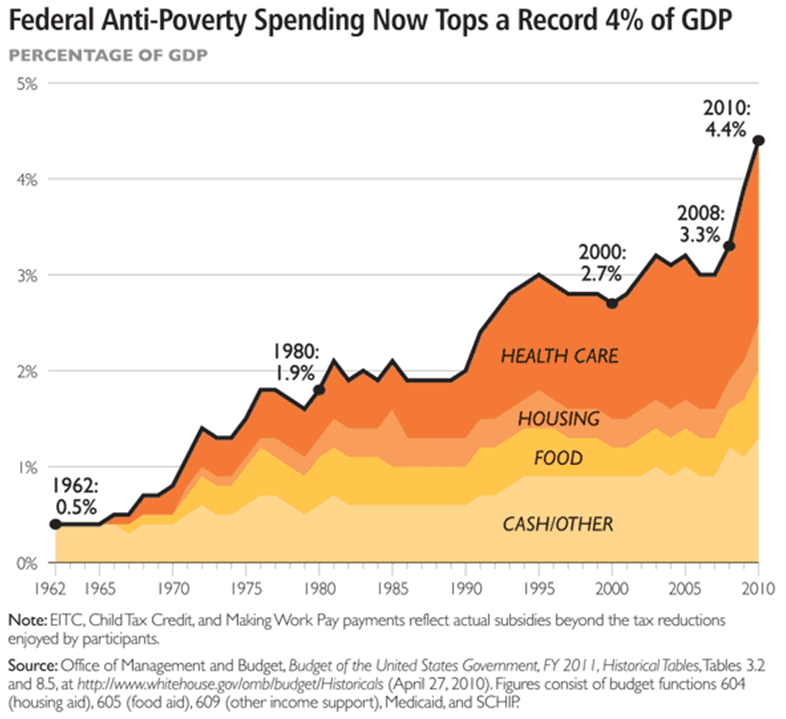
Below are a few more details –
What types of state funded programs potentially have significant overlap in addressable market?
- Medicaid
- Medicaid Transportation Payments
- Low Income Energy Assistance Program Payments
- SNAP (Supplemental Nutrition Assistance Program)
- WIC (Women, Infant & Children Program)
- TANF (Temporary Assistance for Needy Families)
- Child Care Time and Attendance
- SCHIP – State Children’s Health Insurance Program
The tip of the iceberg
In most states, individuals qualifying for food stamps, welfare, Medicaid, etc., must separately apply to different state agencies for these programs. An individual enrolling in multiple programs is just the beginning, as separate departmental processes, eligibility compliance checks and inevitable movement in and out of various programs compound the issue.
Finding an efficient path
As with any inefficient system, waste evokes opportunity. The ability to bundle benefits and combine or transfer the management of those benefits across state agencies will be extremely important in the lowering of administration costs and streamlining the benefits distribution across the states. As states realize the efficiencies gained from this exercise, they will likely invest in solutions that help manage multiple benefit plans and technology that is able to track eligibility and even auto-enroll the appropriate individuals to the appropriate programs. Unfortunately, this is much easier said than done.
Clearing hurdles
The main obstacle in this situation is the lack of administrative and payment capabilities to enable the states to provide the benefits to the eligible consumer (enroll and administer the programs), track usage/transactions, and appropriately distribute the funds. While this will not happen right away, once the public health insurance exchanges are established, it would make a lot of sense to use that exchange infrastructure to allow people to enroll in not only Medicaid, but other government benefits.
This area of compliance in health care is a focus for our team and is rife with opportunities – let us know what you think.
Have a great week.